Obesity and IQ
Previously, I intimated that the connection between obesity and cardiovascular disease and death from such diseases may not be what is commonly believed:
I don’t dispute that overweight and obese people are in poorer health on average, and perhaps do have shorter lives. However, I don’t think it’s at all clear that this is caused by the obesity. It is quite likely, given what we know, that the poorer health results from a higher mutational burden in the overweight (i.e. genetic load), which contributes to both the obesity and the poor health.
…
In any case, impact from obesity on say cardiovascular health fairly small, less than a factor of two, which, for a wholly correlation result is pretty weak.
The idea is that people who are in poorer health have all around poorer genetic quality – in other words, they tend to have higher levels of genetic load (see here at West Hunter, or my HBD Fundamentals page for some discussion on genetic load). And thanks to pleiotropy – that is, genes that impact multiple systems in the body – we tend to see a lot of bad things going together.
Possibly evidencing that in the case of obesity is the connection between obesity and low IQ. It is commonly known that poorer (i.e., stupider) people tend to be fatter. It is commonly believed that this stems from things associated with low IQ, like poor impulse control and low future-time orientation, and indeed those things likely play a role. But it’s telling to see just how stark the relationship is.
Satoshi Kanazawa (who, despite the removal of his Big Think page, still very much publishes; see his website) did just that. Looking at a nationally representative primarily White British sample (n just under 10,000 in the last waves, 97% White), he found that IQ measured in childhood excellently predicts obesity at age 51:
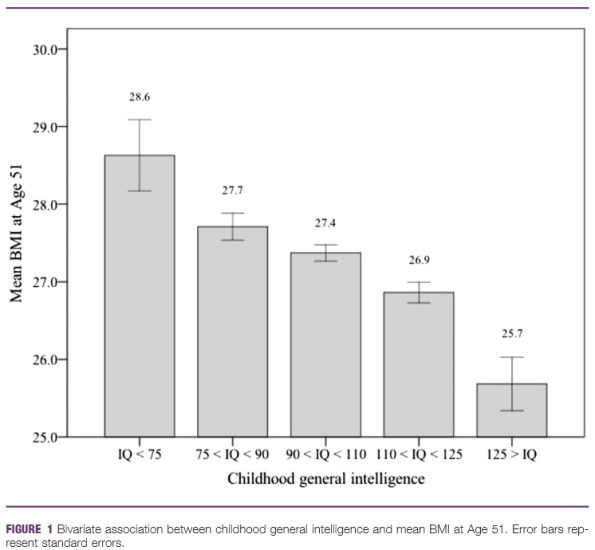
We see a steady drop in average body mass index (BMI) as IQ rises.
This really does seem to turn the conventional wisdom on its head. We know that low-IQ individuals are in poorer health and live shorter lives than do higher IQ individuals. Hence, one cannot help but wonder if the associations between obesity and poor health and cardiovascular risks stems entirely from low IQ.
The association between health and IQ is quite strong, and there is evidence that suggests that it stems not just from the fact that high-IQ individuals take better care of themselves. Higher-IQ individuals just appear to be all around “healthier”, on average, than their lower-IQ counterparts.
IQ is a huge target for genetic load, thanks to the number of genes involved in the brain. Most of the within-population variance in IQ likely stems from overall levels of these deleterious mutations. An individual with a large amount of genetic load is likely to demonstrate fitness deficits in a wide variety of systems. We see this with physical attractiveness, as there is a positive relationship between IQ and attractiveness. We also see this between IQ and height, as taller people are more intelligent on average. Indeed, a recent model indicated that pleiotropy is likely in good part responsible for the connection between height and IQ.
In fact, it has been said that – at least within a population – there aren’t so much “genes for intelligence” as there are “genes for stupidity“. That is, much of variation in IQ stems from these deleterious mutations, each one individually rare and of typically weak effect, but collectively powerful to the hapless soul that happens to have lot of them.
Obesity appears to be somewhat similar. Many of the identified genes that appear to influence obesity seem to operate in the brain, perhaps indicative of the pleiotropic nature of the genetic roots of both low IQ and obesity. (Edit: See this paper by Tyler, Asselbergs, Williams, and Moore (2009) for a technical discussion on the nature of pleiotropy and epistasis.)
Hence, we may be looking at the wrong place when looking at the somewhat poorer outcomes of obese people, and indeed might be foolish to assume that these are outcomes are everybody’s problem; they are primarily a low-IQ problem. I proposed a test that – while not being definitive – might shed some light on this:
A simple test would be [to] compare the health of obese people to thinner people controlling for IQ (a good proxy for genetic load). I’d wager that the ill effects are significantly attenuated.
This would determine which of the two factors – obesity or IQ – had the stronger “impact” (remember, this would be correlational) on negative health outcomes. If it turned out that it was IQ, then it would be much harder to seriously assume that obese people would live longer if they simply lost weight. I look forward to such a study.
Edit: (I forgot to add this when I wrote the post) Kanazawa also noted the same in his paper:
One alternative explanation for the significantly negative association between childhood intelligence and obesity is the ‘‘general fitness factor’’ approach (26), which suggests that both higher intelligence and health (including the ability to stay within the normal weight range) reflect underlying genetic quality. In this context, it is interesting to note that general intelligence is significantly positively associated with BMI at Age 7 … and at Age 11 … and it is not correlated with BMI at Age 16 … In other words, general intelligence is significantly negatively associated with BMI only in adulthood … when individuals have complete control over what to eat and not to eat
The study randomly assigned 5,145 overweight or obese people with Type 2 diabetes to either a rigorous diet and exercise regimen or to sessions in which they got general health information. The diet involved 1,200 to 1,500 calories a day for those weighing less than 250 pounds and 1,500 to 1,800 calories a day for those weighing more. The exercise program was at least 175 minutes a week of moderate exercise.
But 11 years after the study began, researchers concluded it was futile to continue — the two groups had nearly identical rates of heart attacks, strokes and cardiovascular deaths.
[…]
But the outcome is clear, said Dr. David Nathan, a principal investigator and director of the Diabetes Center at Massachusetts General Hospital. “We have to have an adult conversation about this,” he said. “This was a negative result.”
This strongly supports an earlier proposition of mine, that assuming that promoting diet and exercise will ameliorate cardiovascular risk is foolhardy. At least in this group, it did not. Sure, one could argue that these patients were already diabetic, and hence maybe the damage was already done, but, I’m not holding my breath on this one.
In the end, the problems of obesity and cardiovascular disease may just be something we just need to learn to live with – a serenity moment.
Edit, 2/11/15: See also this study by Kanazawa (Intelligence and obesity: which way does the causal direction go?, 2014), which reviews other studies which replicate the findings of this one.
40 Comments
Leave a CommentTrackbacks
- Dark Enlightenment News from Around the Web | Occam's Razor
- IQ and Death | JayMan's Blog
- linkfest – 05/05/13 | hbd* chick
- PC Thought Police go after Geoffrey Miller | Occam's Razor
- 100 Blog Posts – A Reflection on HBD Blogging And What Lies Ahead | JayMan's Blog
- Obese Woman = Gave Up? - clothes, shoes, hair care, skin care, makeup, designers... - Page 3 - City-Data Forum
- Even George W. Bush Has Heart Disease | JayMan's Blog
- Jayman’s blog posts on health | Lion of the Blogosphere
- Muscle and IQ | Lion of the Blogosphere
- Trans Fat Hysteria and the Mystery of Heart Disease | JayMan's Blog
- IQ & weight/height ratio | Brain Size
- Further implications of hippocampal theory | evolutionistx
- アメリカのエリート層にはデブがいない法則について | 最強の日本人
- Why People Are Getting Fatter: Reconciling Genes with Environment - My Blog







Really great post. (BTW, I seem to have changed monikers, from e to Amber. Carry on.)
PS: I know people gain weight with age, but Jesus, I’d need to weigh 140 pounds to have a BMI of 25! I’ve only weighed that much when I gained 50 lbs gorging on poptarts during pregnancy. (Not something I recommend.)
Thanks, and noted. 😉
I didn’t realise Kanazawa had been dismissed from Big Think. I guess the standards are much higher for those who aren’t politically correct.
Is Big Think like TED? I’ve noticed TED videos are getting fluffier and fluffier all the time. And Big Think has Henry Rollins pontificating about something or other. Henry Rollins? Really?
The orthodoxy is getting suffocating. Their house of cards is falling (see: http://www.nature.com/news/disputed-results-a-fresh-blow-for-social-psychology-1.12902) and yet they still have the galls to censor those that would try and understand these things. I secretly think that they just don’t want to give up on being able to call people fat and stupid.
Did you see this interesting study: http://johnhawks.net/weblog/reviews/health/type-2-diabetes-study-stopped-2012.html ?
No I didn’t. Great find! I’m going to update the post accordingly.
Great post and updates. Serenity indeed; I’m reminded of a Scripture (I know you’re not religious, but here it is):
“For bodily exercise profiteth little, but godliness is profitable unto all things, having promise of the life that now is, and of that which is to come” (1 Timothy 4:8)
The evidence also demonstrates the futility of certain policies (e.g. the failed NYC large soda ban, school lunch reforms, junk food “taxes,” etc.) meant to combat obesity…
Thanks.
Yup…
“The evidence also demonstrates the futility of certain policies (e.g. the failed NYC large soda ban, school lunch reforms, junk food “taxes,” etc.) meant to combat obesity…”
Those things are just beginning to be implemented, very little and very slowly. At least 1 decade from now is when we can begin to see if they help or not.
While you do have a point regarding long-term effects of such interventions (and indeed, such effects are what one should look for), my contention is that bans won’t necessarily stop people from consuming (e.g. those who really want to eat/drink large and/or “junky” portions post-ban might get their fill with multiple servings of smaller portions and thus eat/drink more than they would’ve with one large portion). Things like moderation, willingness to diet/exercise consistently, etc. require degrees of discipline; I’m not convinced bans or other restrictions mediate such discipline.
“Previously hunter-gatherers ate a lot more meat. ”
And fruits, and veggies, and leaves, and nuts and seeds. In fact humans in tropical and sub-tropical regions ate mostly all of that, along with insects, lizards, and small animals. Big game was occasional.
First let me mention that I’ve lost 24 pounds since the New Year and I’m feeling smarter every day.
This discussion doesn’t seem to aware of the current cultural context. Obesity is not what it once was. Metabolic syndrome is now epidemic. Most people believe it is because of refined sugars and starches. About six or seven thousand years ago, agriculture changed our diet. About thirty years ago the food industry changed it again. I imagine that with the Neolithic revolution many human strains died out because they couldn’t adapt to the new grain based diet. Previously hunter-gatherers ate a lot more meat. Now it looks as if we are being confronted with another dietary revolution.
So I wonder if in the middle of this rapid change if some of this genetic hypothesizing isn’t a bit premature?
I imagine that there are fat guys waddling around today who had they been born at the time of the Founding Fathers would not have been fat at all. Farmers then ate prodigious amounts of food in order to fuel their 16 hour work days. Yet they were lean. Today that identical genotype with plenty of Coca-Cola and Cheetos makes for a Type II Diabetes diagnosis. If that is so what does ‘genetic load’ mean?
When you focus on genetic links you imply genetic remedies. But there’s a excellent chance that obesity is just a passing phenomenon that will be soon corrected by simple dietary reforms. Some of them are obvious. Outlaw refined sugar. Stop adding gluten to other products. There are essential amino acids and essential fats. There are no essential sugars. We need to learn to react with horror to the very idea of ‘comfort foods’. Or maybe I’m wrong. But the obesity epidemic is new and therefore almost certainly environmental not genetic.
I’m also troubled by the vagueness of the analysis. Obesity is not completely understood but certain aspects are known. Things like Leptin, insulin, and brown fat are important and all of these presumably have genetic variations. But instead of an analysis that mentions any of the known factors in obesity we get a lot of vague speculation about largely undefined concepts like genetic burden. It reminds me of nineteenth century concepts like ‘vital force’.
Albertosaurus
Albertosaurus, I, too, have experienced the effects of different diets. The pregnancies where I ate ‘standard American’ diets resulted in far more weight gain and bigger babies than the pregnancy in which I ate vegetables and avoided refined carbs.
But after birth, the kids’ natural inclinations toward food kicked in; the biggest baby is now proportionately the smallest, the smallest baby now proportionately the biggest (probably won’t last, though, as the middle kid has the most affection for ice cream.)
In short, shit is complicated, and our diets have definitely changed radically, but how our bodies process our diets, why I have never needed to diet and weigh ‘naturally’ under a hundred pounds and my kids are all also very thin, while someone of the same height exposed to the same foods weighs 150 lbs and is constantly trying to diet and has similarly large children, is probably at least somewhat influenced by our underlying genetics.
Good for you! (Probably the placebo effect though.)
Indeed. I covered all that:
Fun Facts About Obesity
No, variation in obesity is still heritable. Indeed, new environments can increase the heritability in traits (by making genetic variation more important to trait expression, for example).
As well, cardiovascular risk appears to be heritable. Figuring out the connections and causal relationships is quite important.
There was a paper that claimed that health during Victorian-era Britain was much better for Anglos today. They were thinner and purported had less cardiovascular disease. I am doubtful because I am suspect of the reliability of 19th century medicine.
Change the environment, you change the phenotypes. See above.
Not necessarily.
Contrary to what Heartiste might claim, you might find that there is nothing simple about such reforms.
I’m trying to shed light on the assumed relationship between obesity and poor health and cardiovascular risk. If one doesn’t cause the other, but rather, both are symptoms of the same common genetic roots, that changes the game when it comes to the proper guidelines for treating these issues – which might turn out to be nothing.
I think the solution is simple. The brain itself burns calories. Busier brains burn far more calories.
http://io9.com/5920970/how-many-calories-does-thinking-burn
“Now the brain, all on its own, burns only about a tenth of a calorie per minute. Percentage-wise, that’s very high for a resting body tissue. When the brain kicks into gear, though, it really gets impressive. When actively thinking about things, the brain can kick it up to burning a calorie and a half per minute.”
A calorie and a half per minute! That is 90 calories per hour! Hour after hour, people with bigger, busier brains are burning way more calories. Meanwhile the brain that is doing nothig burns six calories per hour. That is all the explanation you need.
Another thing (I may have mentioned it before) is that cancer appears largely unrelated to IQ. It’s interesting because IQ is linked to lots of health behaviors. People love to think that health behaviors will fix everything but smart people eat their vegetables and get cancer anyway. This is slightly off topic but I just wanted to point out that no one is talking about how small the effects of health behaviors for cancer must be if IQ can’t mediate them. This isn’t getting any headlines. Maybe the same situation for cardiovascular disease, although in that case their is an actual correlation so they jump to the conclusion that health behaviors must be the answer.
http://www.ncbi.nlm.nih.gov/pubmed/17220284
My cat has a really low IQ. It must have a really high genetic load.
I wanted to hit my weight on an IQ test, but I got fat and dumb. Actually, though, I probably achieved this around the time of my last (teen) test, before I put on serious lard.
Cheap carbs and sugars and just such a massive stimulus/$ compared to anything else in modern society. Combine that with the fact that passive entertainments (like TV) are very cost effective and its not a surprise.
Look I am thin and miserable and can hardly count up to 10 nor read a book, nor write at all, I just know a few words and this is all they are…..
How about a relationship between homosexuality and IQ?
As I understand that you’re speaking of averages and groups, I find this post highly interesting and not at all objectionable, even though I am short, fat and have ADHD along with being gifted 😉
I also added to your publication of information on childhood obesity that I found in a blog http://www.clinique-obesite.com/la-sleeve.html
I would argue obesity in childhood probably correlates more with the IQ of the parents than the child. But of course the apple dosen’t fall far from the tree. As for mutational load not sure how much that correlates.